New Brunswick, N.J., July 7, 2021 – Researchers at Rutgers Cancer Institute of New Jersey, Rutgers New Jersey Medical School (NJMS) and the Center for Theoretical Biological Physics (CTBP) at Rice University in Houston, Texas, have demonstrated that a technology with favorable biological attributes known as phage display could be a viable platform for the development of new vaccines to protect against COVID-19. Findings from the proof-of-concept work were published online in the Proceedings of the National Academy of Sciences (PNAS) journal (DOI: 2105739118).
Currently approved vaccines against COVID-19 worldwide include mRNA-based vaccines, non-replicating adenovirus vaccines, and an inactivated SARS-CoV-2 vaccine among others. While being broadly effective, these vaccine types suffer many challenges, particularly in rapid large-scale production and distribution, with the requirement for strict storage at low-temperatures (a so-called “cold chain”), use of needles for administration, and a currently unknown ability to confer long-term protection in the face of emerging viral variants.
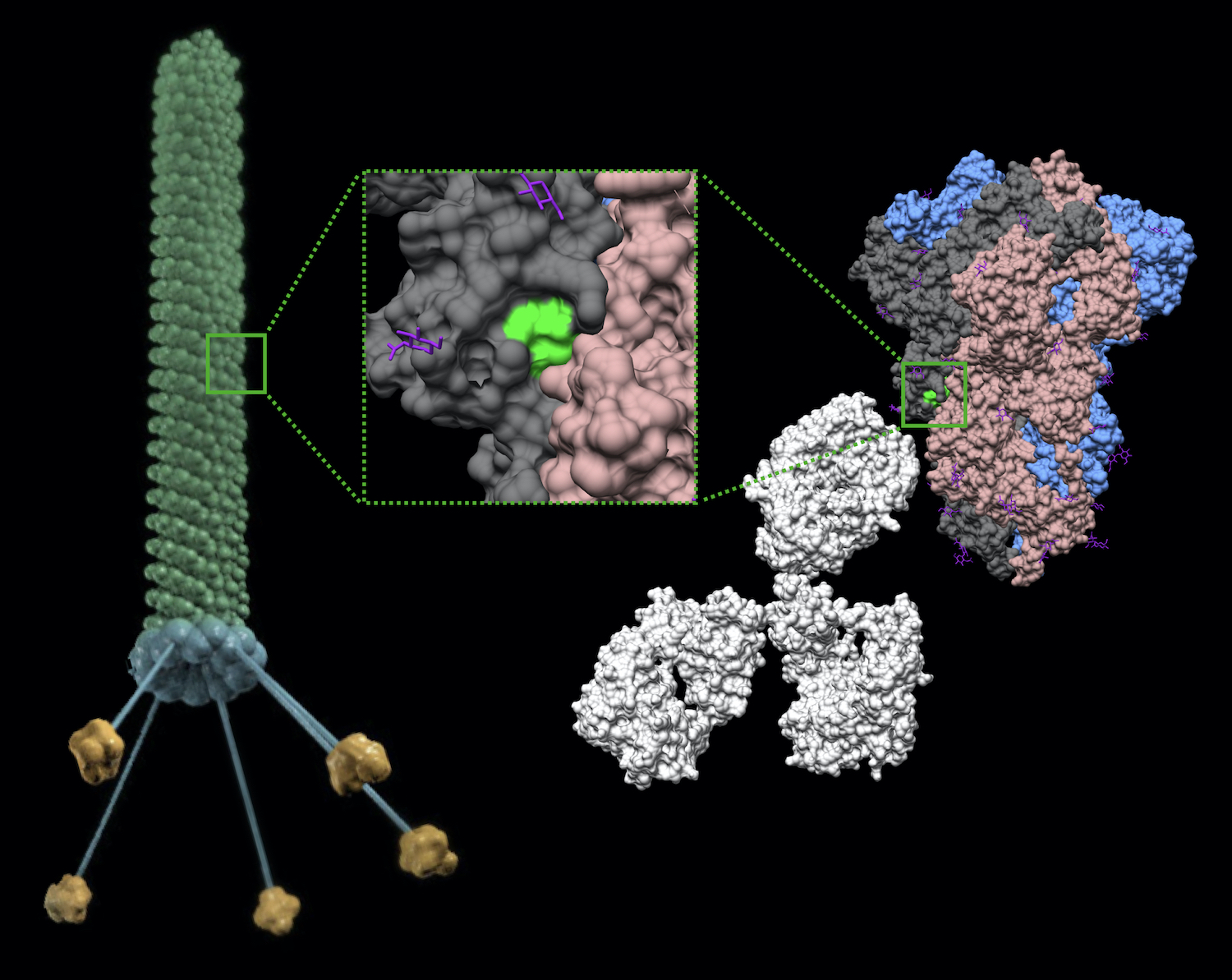
Bacteriophage (phage) are viruses that infect only bacteria yet can serve as powerful tools for translational medicine in humans. In this rendition, a phage particle displays a region of the SARS-CoV-2 Spike protein that retains a near-native structural conformation. Administration of this phage in mice induces a systemic immune response against the Spike protein. This versatile technology serves as a first step towards developing cost-effective and easy-to-manufacture vaccines for COVID-19 and other infectious agents.
Spike protein trimer (PDB ID: 6ZP0) (Xiong et al., 2020) (DOI: 10.1038/s41594-020-0478-5) and IgG antibody (PDB ID: 1IGT) (Harris et al., 1997) (DOI: 10.1021/bi962514+) were depicted using UCSF Chimera.
(Photo credit:) Christopher Markosian/Daniela Staquicini/Rutgers Cancer Institute of New Jersey/Rutgers New Jersey Medical School
One completely unexplored alternative is the design and development of phage display-based vaccines, which represent an inexpensive and versatile tool for large-scale immunization. Bacteriophage (phage) are viruses that naturally only infect bacteria, thus they are generally considered safe for use in humans. Phage particles are easy to genetically engineer or modify and produce in large quantities; capable of stimulating both cellular and humoral immunity; and are stable under harsh environmental conditions (pH and temperature).
In this study, the authors developed two independent phage display-based vaccination approaches against SARS-CoV-2, the virus that causes COVID-19. The first is a peptide-directed phage particle that can be administered in an aerosolized form by inhalation. It is engineered with an epitope from the SARS-CoV-2 spike (S) protein together with a small ligand peptide to ensure it crossed from the lungs into the systemic circulation, where it produced a strong antibody response in mice. In the second approach, they engineered chimeric adeno-associated virus-phage (AAVP) particles to deliver the gene encoding for the entire S protein, which also stimulated a systemic and specific antibody response in mice.
This dual proof-of-concept experimentation demonstrates that phage display-based vaccine approaches are versatile platforms that could be used for rapid production of COVID-19 vaccines that are cost-effective, needle-free, and can be safely stored long-term at room temperature. Combined with a theoretical structural biology approach to identify effective epitopes, this work provides a new framework for vaccine development. Further research and development of prototype COVID-19 investigational vaccines and alternative methods of application such as inhalation are ongoing.
“In the development of new vaccination strategies, the structure and strength of the local healthcare system is a key consideration. As such the global COVID-19 pandemic has raised awareness of public health inequity and the need for a rapid and accessible immunization process. In this context, the favorable biological attributes of phage particles might represent a potentially practical yet affordable alternative,” shares the study’s senior author Renata Pasqualini, PhD, resident member of Rutgers Cancer Institute and professor and founding chief of the Division of Cancer Biology, Department of Radiation Oncology at Rutgers NJMS.
The study’s other senior author, Wadih Arap, MD, PhD, director of Rutgers Cancer Institute at University Hospital Newark and professor and chief of the Division of Hematology/Oncology, Department of Medicine, Rutgers NJMS, notes, “Bacteriophage-based therapy has a long and rich history in medicine because native phage particles are not infectious to human cells. The new appeal here is that we were able to modify the phage particles so that they may now target cell surface receptors; moreover, another potential application of this platform technology is the possibility of an inhaled vaccine administration.”
"One of the challenges in designing these vaccines is that, when we insert the different SARS-CoV-2 spike epitopes into the phage particles, the structure of these peptides needs to stay intact as in the original protein. In this collaboration, we demonstrated that the epitopes that show the smallest deviations from the original structure are the ones most effective in creating immune protection,” adds José N. Onuchic, PhD, Harry C. and Olga K. Wiess Chair of Physics and professor of chemistry and biosciences at Rice University, who is a corresponding author on the study with Drs. Arap and Pasqualini. “This initial success allows us to create a synergistic theoretical/experimental framework to discover new possible epitopes to improve these vaccines not only for SARS-CoV-2 but for other diseases as well," adds Dr. Onuchic, who is also co-director of the CTBP at Rice University.
PNAS paper video produced by Rice University. Credit: Paul Whitford and Esteban Dodero-Rojas.
This video illustrates how theoretical models and simulations can be used to guide the development of COVID-19 vaccines. As depicted in the movie, Staquicini et al. (DOI: 2105739118) used all-atom simulations to identify promising epitopes, which were engineered into phage particles used to generate an immune response against COVID-19. This strategy may allow for rapid development and deployment of novel vaccines that are customized to target any number of emerging COVID-19 variants.
This work was supported in part by core services from the Rutgers Cancer Institute of New Jersey Cancer Center Support Grant (P30CA072720); the RCSB Protein Data Bank, which is jointly funded by the National Science Foundation (DBI-1832184); the U.S. Department of Energy (DE-SC0019749), and the National Cancer Institute, National Institute of Allergy and Infectious Diseases, and National Institute of General Medical Sciences of the National Institutes of Health (R01GM133198). Work at the Center for Theoretical Biological Physics was supported by the National Science Foundation (grants PHY-2019745, CHE-1614101 and PHY-1522550) and the Welch Foundation (grant C-1792). Additional funding information and author disclosures can be found here. (DOI: 2105739118).
About Rutgers Cancer Institute of New Jersey
As New Jersey’s only National Cancer Institute-designated Comprehensive Cancer Center, Rutgers Cancer Institute, together with RWJBarnabas Health, offers the most advanced cancer treatment options including bone marrow transplantation, proton therapy, CAR T-cell therapy and complex surgical procedures. Along with clinical trials and novel therapeutics such as precision medicine and immunotherapy – many of which are not widely available – patients have access to these cutting-edge therapies at Rutgers Cancer Institute of New Jersey in New Brunswick, Rutgers Cancer Institute of New Jersey at University Hospital in Newark, as well as through RWJBarnabas Health facilities. To make a tax-deductible gift to support Rutgers Cancer Institute of New Jersey, call 848-932-8013 or visit www.cinj.org/giving.
About Rutgers New Jersey Medical School
Founded in 1954, Rutgers New Jersey Medical School is the oldest school of medicine in the state. Today it is part of Rutgers, The State University of New Jersey and graduates approximately 170 physicians a year. In addition to providing the MD degree, the school offers MD/PhD, MD/MPH and MD/MBA degrees through collaborations with other institutions of higher education. Dedicated to excellence in education, research, clinical care and community outreach, the medical school comprises 20 academic departments and works with several healthcare partners, including its principal teaching hospital, University Hospital. Its faculty consists of numerous world-renowned scientists and many of the region’s “top doctors.” Home to the nation’s oldest student-run clinic, New Jersey Medical School hosts more than 50 centers and institutes, including the Public Health Research Institute Center, the Global Tuberculosis Institute and the Neurological Institute of New Jersey. For more information please visit: njms.rutgers.edu.
About Rice University
Located on a 300-acre forested campus in Houston, Rice University is consistently ranked among the nation’s top 20 universities by U.S. News & World Report. Rice has highly respected schools of Architecture, Business, Continuing Studies, Engineering, Humanities, Music, Natural Sciences and Social Sciences and is home to the Baker Institute for Public Policy. With 3,978 undergraduates and 3,192 graduate students, Rice’s undergraduate student-to-faculty ratio is just under 6-to-1. Its residential college system builds close-knit communities and lifelong friendships, just one reason why Rice is ranked No. 1 for lots of race/class interaction and No. 1 for quality of life by the Princeton Review. Rice is also rated as a best value among private universities by Kiplinger’s Personal Finance.
###
For journalists – contact:
Krista Didzbalis
Media Relations Assistant, Rutgers Cancer Institute
908-812-6114
krista.didzbalis@rutgers.edu
Mike Williams
Senior Media Relations Specialist, Rice University
713-348-6728
mikewilliams@rice.edu
For patient appointments/inquiries at Rutgers Cancer Institute – contact:
844-CANCERNJ (844-226-2376)